[1] Dillon J. F. (2004). Hepatitis C: What is the best treatment?. Journal of viral hepatitis, 11 Suppl 1, 23–27. https://doi.org/10.1111/j.1365-2893.2004.00573.x
[2] Campos, M. C., Nery, T., Starke, A. C., de Bem Alves, A. C., Speck, A. E., & S Aguiar, A. (2022). Post-viral fatigue in COVID-19: A review of symptom assessment methods, mental, cognitive, and physical impairment. Neuroscience and biobehavioral reviews, 142, 104902. https://doi.org/10.1016/j.neubiorev.2022.104902
[3] Krishnan, K., Lin, Y., Prewitt, K. M., & Potter, D. A. (2022). Multidisciplinary Approach to Brain Fog and Related Persisting Symptoms Post COVID-19. Journal of health service psychology, 48(1), 31–38. https://doi.org/10.1007/s42843-022-00056-7
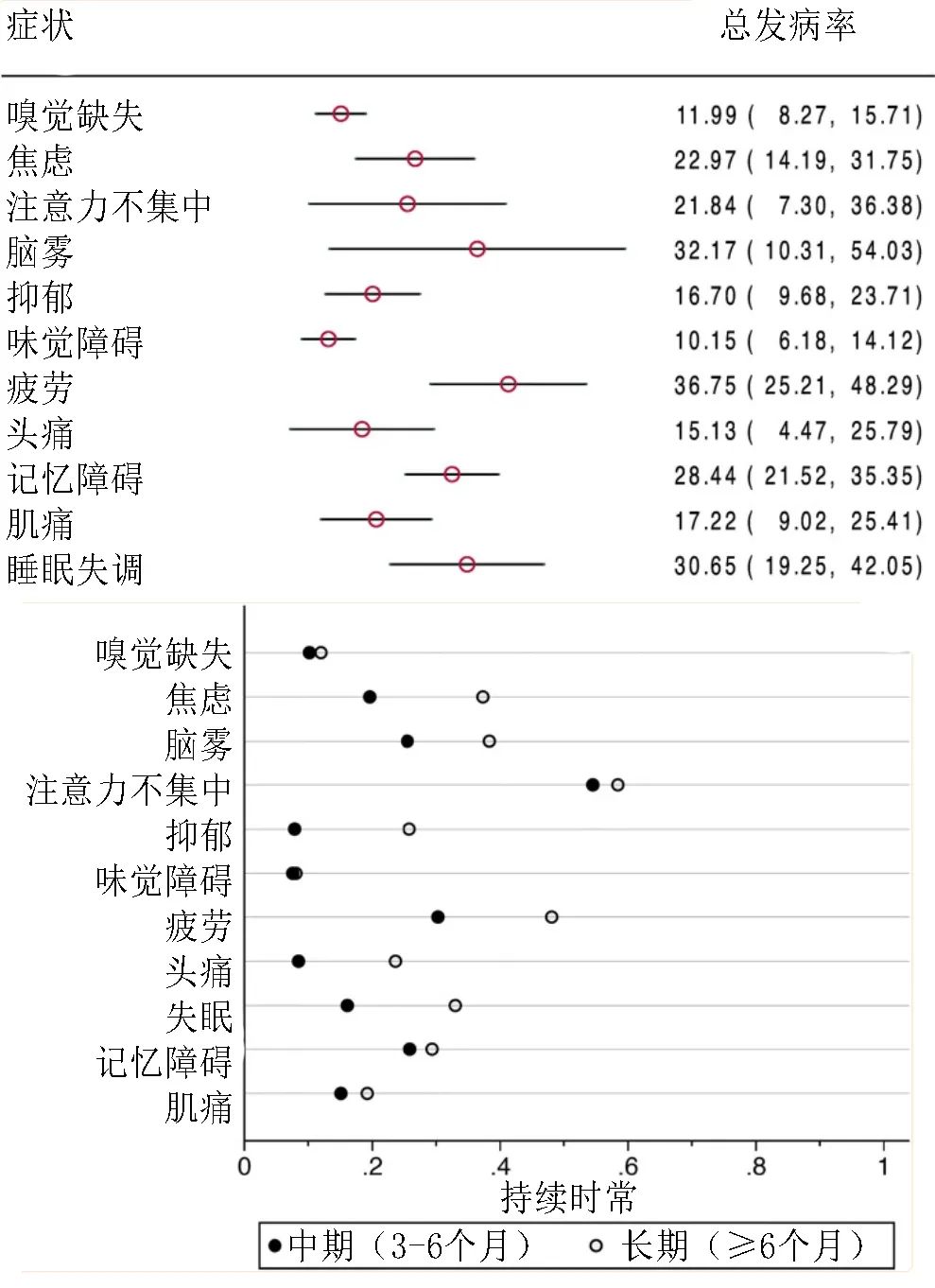
[4] Premraj, L., Kannapadi, N. V., Briggs, J., Seal, S. M., Battaglini, D., Fanning, J., Suen, J., Robba, C., Fraser, J., & Cho, S. M. (2022). Mid and long-term neurological and neuropsychiatric manifestations of post-COVID-19 syndrome: A meta-analysis. Journal of the neurological sciences, 434, 120162. https://doi.org/10.1016/j.jns.2022.120162
[5] Peluso, M. J., Lu, S., Tang, A. F., Durstenfeld, M. S., Ho, H. E., Goldberg, S. A., Forman, C. A., Munter, S. E., Hoh, R., Tai, V., Chenna, A., Yee, B. C., Winslow, J. W., Petropoulos, C. J., Greenhouse, B., Hunt, P. W., Hsue, P. Y., Martin, J. N., Daniel Kelly, J., Glidden, D. V., … Henrich, T. J. (2021). Markers of Immune Activation and Inflammation in Individuals With Postacute Sequelae of Severe Acute Respiratory Syndrome Coronavirus 2 Infection. The Journal of infectious diseases, 224(11), 1839–1848. https://doi.org/10.1093/infdis/jiab490
[6] Chen, C., Haupert, S. R., Zimmermann, L., Shi, X., Fritsche, L. G., & Mukherjee, B. (2022). Global Prevalence of Post-Coronavirus Disease 2019 (COVID-19) Condition or Long COVID: A Meta-Analysis and Systematic Review. The Journal of infectious diseases, 226(9), 1593–1607. https://doi.org/10.1093/infdis/jiac136
[7] Subramanian, A., Nirantharakumar, K., Hughes, S., Myles, P., Williams, T., Gokhale, K. M., Taverner, T., Chandan, J. S., Brown, K., Simms-Williams, N., Shah, A. D., Singh, M., Kidy, F., Okoth, K., Hotham, R., Bashir, N., Cockburn, N., Lee, S. I., Turner, G. M., Gkoutos, G. V., … Haroon, S. (2022). Symptoms and risk factors for long COVID in non-hospitalized adults. Nature medicine, 28(8), 1706–1714. https://doi.org/10.1038/s41591-022-01909-w
[8] Mantovani, A., Morrone, M. C., Patrono, C., Santoro, M. G., Schiaffino, S., Remuzzi, G., Bussolati, G., & Covid-19 Commission of the Accademia Nazionale dei Lincei (2022). Long Covid: where we stand and challenges ahead. Cell death and differentiation, 29(10), 1891–1900. https://doi.org/10.1038/s41418-022-01052-6
[9] Helms, J., Kremer, S., Merdji, H., Clere-Jehl, R., Schenck, M., Kummerlen, C., Collange, O., Boulay, C., Fafi-Kremer, S., Ohana, M., Anheim, M., & Meziani, F. (2020). Neurologic Features in Severe SARS-CoV-2 Infection. The New England journal of medicine, 382(23), 2268–2270. https://doi.org/10.1056/NEJMc2008597
[10] Vasek, M. J., Garber, C., Dorsey, D., Durrant, D. M., Bollman, B., Soung, A., Yu, J., Perez-Torres, C., Frouin, A., Wilton, D. K., Funk, K., DeMasters, B. K., Jiang, X., Bowen, J. R., Mennerick, S., Robinson, J. K., Garbow, J. R., Tyler, K. L., Suthar, M. S., Schmidt, R. E., … Klein, R. S. (2016). A complement-microglial axis drives synapse loss during virus-induced memory impairment. Nature, 534(7608), 538–543. https://doi.org/10.1038/nature18283
[11] Heneka, M. T., Golenbock, D., Latz, E., Morgan, D., & Brown, R. (2020). Immediate and long-term consequences of COVID-19 infections for the development of neurological disease. Alzheimer's research & therapy, 12(1), 69. https://doi.org/10.1186/s13195-020-00640-3
[12] Semmler, A., Widmann, C. N., Okulla, T., Urbach, H., Kaiser, M., Widman, G., Mormann, F., Weide, J., Fliessbach, K., Hoeft, A., Jessen, F., Putensen, C., & Heneka, M. T. (2013). Persistent cognitive impairment, hippocampal atrophy and EEG changes in sepsis survivors. Journal of neurology, neurosurgery, and psychiatry, 84(1), 62–69. https://doi.org/10.1136/jnnp-2012-302883
[13] Thakur, K. T., Miller, E. H., Glendinning, M. D., Al-Dalahmah, O., Banu, M. A., Boehme, A. K., Boubour, A. L., Bruce, S. S., Chong, A. M., Claassen, J., Faust, P. L., Hargus, G., Hickman, R. A., Jambawalikar, S., Khandji, A. G., Kim, C. Y., Klein, R. S., Lignelli-Dipple, A., Lin, C. C., Liu, Y., … Canoll, P. (2021). COVID-19 neuropathology at Columbia University Irving Medical Center/New York Presbyterian Hospital. Brain : a journal of neurology, 144(9), 2696–2708. https://doi.org/10.1093/brain/awab148
[14] Zhou, H., Lu, S., Chen, J., Wei, N., Wang, D., Lyu, H., Shi, C., & Hu, S. (2020). The landscape of cognitive function in recovered COVID-19 patients. Journal of psychiatric research, 129, 98–102. https://doi.org/10.1016/j.jpsychires.2020.06.022
[15] Chen, Y., Yang, W., Chen, F., & Cui, L. (2022). COVID-19 and cognitive impairment: neuroinvasive and blood‒brain barrier dysfunction. Journal of neuroinflammation, 19(1), 222. https://doi.org/10.1186/s12974-022-02579-8
[16] Brun, G., Hak, J. F., Coze, S., Kaphan, E., Carvelli, J., Girard, N., & Stellmann, J. P. (2020). COVID-19-White matter and globus pallidum lesions: Demyelination or small-vessel vasculitis?. Neurology(R) neuroimmunology & neuroinflammation, 7(4), e777. https://doi.org/10.1212/NXI.0000000000000777
[17] Ystad, M., Hodneland, E., Adolfsdottir, S., Haász, J., Lundervold, A. J., Eichele, T., & Lundervold, A. (2011). Cortico-striatal connectivity and cognition in normal aging: a combined DTI and resting state fMRI study. NeuroImage, 55(1), 24–31. https://doi.org/10.1016/j.neuroimage.2010.11.016
[18] Lu, Y., Li, X., Geng, D., Mei, N., Wu, P. Y., Huang, C. C., Jia, T., Zhao, Y., Wang, D., Xiao, A., & Yin, B. (2020). Cerebral Micro-Structural Changes in COVID-19 Patients - An MRI-based 3-month Follow-up Study. EClinicalMedicine, 25, 100484. https://doi.org/10.1016/j.eclinm.2020.100484
[19] Moghimi, N., Di Napoli, M., Biller, J., Siegler, J. E., Shekhar, R., McCullough, L. D., Harkins, M. S., Hong, E., Alaouieh, D. A., Mansueto, G., & Divani, A. A. (2021). The Neurological Manifestations of Post-Acute Sequelae of SARS-CoV-2 infection. Current neurology and neuroscience reports, 21(9), 44. https://doi.org/10.1007/s11910-021-01130-1
[20] Newhouse, A., Kritzer, M. D., Eryilmaz, H., Praschan, N., Camprodon, J. A., Fricchione, G., & Chemali, Z. (2022). Neurocircuitry Hypothesis and Clinical Experience in Treating Neuropsychiatric Symptoms of Postacute Sequelae of Severe Acute Respiratory Syndrome Coronavirus 2. Journal of the Academy of Consultation-Liaison Psychiatry, 63(6), 619–627. https://doi.org/10.1016/j.jaclp.2022.08.007
[21] Hosp, J. A., Dressing, A., Blazhenets, G., Bormann, T., Rau, A., Schwabenland, M., Thurow, J., Wagner, D., Waller, C., Niesen, W. D., Frings, L., Urbach, H., Prinz, M., Weiller, C., Schroeter, N., & Meyer, P. T. (2021). Cognitive impairment and altered cerebral glucose metabolism in the subacute stage of COVID-19. Brain : a journal of neurology, 144(4), 1263–1276. https://doi.org/10.1093/brain/awab009
[22] Dangayach, N. S., Newcombe, V., & Sonnenville, R. (2022). Acute Neurologic Complications of COVID-19 and Postacute Sequelae of COVID-19. Critical care clinics, 38(3), 553–570. https://doi.org/10.1016/j.ccc.2022.03.002
[23] Stefanou, M. I., Palaiodimou, L., Bakola, E., Smyrnis, N., Papadopoulou, M., Paraskevas, G. P., Rizos, E., Boutati, E., Grigoriadis, N., Krogias, C., Giannopoulos, S., Tsiodras, S., Gaga, M., & Tsivgoulis, G. (2022). Neurological manifestations of long-COVID syndrome: a narrative review. Therapeutic advances in chronic disease, 13, 20406223221076890. https://doi.org/10.1177/20406223221076890
[24] Bisaccia, G., Ricci, F., Recce, V., Serio, A., Iannetti, G., Chahal, A. A., Ståhlberg, M., Khanji, M. Y., Fedorowski, A., & Gallina, S. (2021). Post-Acute Sequelae of COVID-19 and Cardiovascular Autonomic Dysfunction: What Do We Know?. Journal of cardiovascular development and disease, 8(11), 156. https://doi.org/10.3390/jcdd8110156
[25] Mathern, R., Senthil, P., Vu, N., & Thiyagarajan, T. (2022). Neurocognitive Rehabilitation in COVID-19 Patients: A Clinical Review. Southern medical journal, 115(3), 227–231. https://doi.org/10.14423/SMJ.0000000000001371
[26] Cardinali, D. P., Brown, G. M., & Pandi-Perumal, S. R. (2022). Possible Application of Melatonin in Long COVID. Biomolecules, 12(11), 1646. https://doi.org/10.3390/biom12111646
[27] Theoharides, T. C., Cholevas, C., Polyzoidis, K., & Politis, A. (2021). Long-COVID syndrome-associated brain fog and chemofog: Luteolin to the rescue. BioFactors (Oxford, England), 47(2), 232–241. https://doi.org/10.1002/biof.1726
[28] De Luca, P., Camaioni, A., Marra, P., Salzano, G., Carriere, G., Ricciardi, L., Pucci, R., Montemurro, N., Brenner, M. J., & Di Stadio, A. (2022). Effect of Ultra-Micronized Palmitoylethanolamide and Luteolin on Olfaction and Memory in Patients with Long COVID: Results of a Longitudinal Study. Cells, 11(16), 2552. https://doi.org/10.3390/cells11162552
[29] Satoh, T., Trudler, D., Oh, C. K., & Lipton, S. A. (2022). Potential Therapeutic Use of the Rosemary Diterpene Carnosic Acid for Alzheimer's Disease, Parkinson's Disease, and Long-COVID through NRF2 Activation to Counteract the NLRP3 Inflammasome. Antioxidants (Basel, Switzerland), 11(1), 124. https://doi.org/10.3390/antiox11010124