[1]https://mp.weixin.qq.com/s/GB5sAqEITABMC7enbXm5bA
[2]http://www.nhc.gov.cn/xcs/gzzcwj/202211/9bb71c9c7d664fb0bbcd2b3eaaefcf84.shtml
[3]Tregoning, J. S., Flight, K. E., Higham, S. L., Wang, Z., & Pierce, B. F. (2021). Progress of the COVID-19 vaccine effort: viruses, vaccines and variants versus efficacy, effectiveness and escape. Nature reviews. Immunology, 21(10), 626–636. https://doi.org/10.1038/s41577-021-00592-1
[4]http://www.nhc.gov.cn/xcs/yqfkdt/202212/bdf09923a0724760becaa8a775c71a6b.shtml
[5]http://www.yangchun.gov.cn/zxzx/bmtx/content/post_527736.html
[6]Shimabukuro, T. T., Cole, M., & Su, J. R. (2021). Reports of Anaphylaxis After Receipt of mRNA COVID-19 Vaccines in the US-December 14, 2020-January 18, 2021. JAMA, 325(11), 1101–1102. https://doi.org/10.1001/jama.2021.1967
[7]Larson, K. F., Ammirati, E., Adler, E. D., Cooper, L. T., Jr, Hong, K. N., Saponara, G., Couri, D., Cereda, A., Procopio, A., Cavalotti, C., Oliva, F., Sanna, T., Ciconte, V. A., Onyango, G., Holmes, D. R., & Borgeson, D. D. (2021). Myocarditis After BNT162b2 and mRNA-1273 Vaccination. Circulation, 144(6), 506–508. https://doi.org/10.1161/CIRCULATIONAHA.121.055913
[8]Pottegård, A., Lund, L. C., Karlstad, Ø., Dahl, J., Andersen, M., Hallas, J., Lidegaard, Ø., Tapia, G., Gulseth, H. L., Ruiz, P. L., Watle, S. V., Mikkelsen, A. P., Pedersen, L., Sørensen, H. T., Thomsen, R. W., & Hviid, A. (2021). Arterial events, venous thromboembolism, thrombocytopenia, and bleeding after vaccination with Oxford-AstraZeneca ChAdOx1-S in Denmark and Norway: population based cohort study. BMJ (Clinical research ed.), 373, n1114. https://doi.org/10.1136/bmj.n1114
[9]Satija, A., & Hu, F. B. (2018). Plant-based diets and cardiovascular health. Trends in cardiovascular medicine, 28(7), 437–441. https://doi.org/10.1016/j.tcm.2018.02.004
[10]Kim, H., Rebholz, C. M., Hegde, S., LaFiura, C., Raghavan, M., Lloyd, J. F., Cheng, S., & Seidelmann, S. B. (2021). Plant-based diets, pescatarian diets and COVID-19 severity: a population-based case-control study in six countries. BMJ nutrition, prevention & health, 4(1), 257–266. https://doi.org/10.1136/bmjnph-2021-000272
[11]Storz M. A. (2021). Lifestyle Adjustments in Long-COVID Management: Potential Benefits of Plant-Based Diets. Current nutrition reports, 10(4), 352–363. https://doi.org/10.1007/s13668-021-00369-x
[12]Kahleova, H., Levin, S., & Barnard, N. D. (2018). Vegetarian Dietary Patterns and Cardiovascular Disease. Progress in cardiovascular diseases, 61(1), 54–61. https://doi.org/10.1016/j.pcad.2018.05.002
[13]Mello, M. T., Silva, A., Guerreiro, R. C., da-Silva, F. R., Esteves, A. M., Poyares, D., Piovezan, R., Treptow, E., Starling, M., Rosa, D. S., Pires, G. N., Andersen, M. L., & Tufik, S. (2020). Sleep and COVID-19: considerations about immunity, pathophysiology, and treatment. Sleep science (Sao Paulo, Brazil), 13(3), 199–209. https://doi.org/10.5935/1984-0063.20200062
[14]Shillington, K. J., Vanderloo, L. M., Burke, S. M., Ng, V., Tucker, P., & Irwin, J. D. (2022). Not so sweet dreams: adults' quantity, quality, and disruptions of sleep during the initial stages of the COVID-19 pandemic. Sleep medicine, 91, 189–195. https://doi.org/10.1016/j.sleep.2021.02.028
[15]Kim, H., Hegde, S., LaFiura, C., Raghavan, M., Luong, E., Cheng, S., Rebholz, C. M., & Seidelmann, S. B. (2021). COVID-19 illness in relation to sleep and burnout. BMJ nutrition, prevention & health, 4(1), 132–139. https://doi.org/10.1136/bmjnph-2021-000228
[16]Lee, S. W., Lee, J., Moon, S. Y., Jin, H. Y., Yang, J. M., Ogino, S., Song, M., Hong, S. H., Abou Ghayda, R., Kronbichler, A., Koyanagi, A., Jacob, L., Dragioti, E., Smith, L., Giovannucci, E., Lee, I. M., Lee, D. H., Lee, K. H., Shin, Y. H., Kim, S. Y., … Yon, D. K. (2022). Physical activity and the risk of SARS-CoV-2 infection, severe COVID-19 illness and COVID-19 related mortality in South Korea: a nationwide cohort study. British journal of sports medicine, 56(16), 901–912. https://doi.org/10.1136/bjsports-2021-104203
[17]Roviello, V., Gilhen-Baker, M., Vicidomini, C., & Roviello, G. N. (2022). Forest-bathing and physical activity as weapons against COVID-19: a review. Environmental chemistry letters, 20(1), 131–140. https://doi.org/10.1007/s10311-021-01321-9
[18]Nieman, D. C., & Wentz, L. M. (2019). The compelling link between physical activity and the body's defense system. Journal of sport and health science, 8(3), 201–217. https://doi.org/10.1016/j.jshs.2018.09.009
[19]Sallis, R., Young, D. R., Tartof, S. Y., Sallis, J. F., Sall, J., Li, Q., Smith, G. N., & Cohen, D. A. (2021). Physical inactivity is associated with a higher risk for severe COVID-19 outcomes: a study in 48 440 adult patients. British journal of sports medicine, 55(19), 1099–1105. https://doi.org/10.1136/bjsports-2021-104080
[20]Laddu, D. R., Lavie, C. J., Phillips, S. A., & Arena, R. (2021). Physical activity for immunity protection: Inoculating populations with healthy living medicine in preparation for the next pandemic. Progress in cardiovascular diseases, 64, 102–104. https://doi.org/10.1016/j.pcad.2020.04.006
[21]Huang, B., Niu, Y., Zhao, W., Bao, P., & Li, D. (2020). Reduced Sleep in the Week Prior to Diagnosis of COVID-19 is Associated with the Severity of COVID-19. Nature and science of sleep, 12, 999–1007. https://doi.org/10.2147/NSS.S263488
[22]http://www.nhc.gov.cn/wjw/hygq/202101/146c4e7347c0435a82a8178dd76cf280.shtml
[23]Zahedipour, F., Hosseini, S. A., Sathyapalan, T., Majeed, M., Jamialahmadi, T., Al-Rasadi, K., Banach, M., & Sahebkar, A. (2020). Potential effects of curcumin in the treatment of COVID-19 infection. Phytotherapy research : PTR, 34(11), 2911–2920. https://doi.org/10.1002/ptr.6738
[24]Kow, C. S., Ramachandram, D. S., & Hasan, S. S. (2022). The effect of curcumin on the risk of mortality in patients with COVID-19: A systematic review and meta-analysis of randomized trials. Phytotherapy research : PTR, 36(9), 3365–3368. https://doi.org/10.1002/ptr.7468
[25]Thimmulappa, R. K., Mudnakudu-Nagaraju, K. K., Shivamallu, C., Subramaniam, K. J. T., Radhakrishnan, A., Bhojraj, S., & Kuppusamy, G. (2021). Antiviral and immunomodulatory activity of curcumin: A case for prophylactic therapy for COVID-19. Heliyon, 7(2), e06350. https://doi.org/10.1016/j.heliyon.2021.e06350
[26]Di Petrillo, A., Orrù, G., Fais, A., & Fantini, M. C. (2022). Quercetin and its derivates as antiviral potentials: A comprehensive review. Phytotherapy research : PTR, 36(1), 266–278. https://doi.org/10.1002/ptr.7309
[27]Derosa, G., Maffioli, P., D'Angelo, A., & Di Pierro, F. (2021). A role for quercetin in coronavirus disease 2019 (COVID-19). Phytotherapy research : PTR, 35(3), 1230–1236. https://doi.org/10.1002/ptr.6887
[28]Di Pierro, F., Derosa, G., Maffioli, P., Bertuccioli, A., Togni, S., Riva, A., Allegrini, P., Khan, A., Khan, S., Khan, B. A., Altaf, N., Zahid, M., Ujjan, I. D., Nigar, R., Khushk, M. I., Phulpoto, M., Lail, A., Devrajani, B. R., & Ahmed, S. (2021). Possible Therapeutic Effects of Adjuvant Quercetin Supplementation Against Early-Stage COVID-19 Infection: A Prospective, Randomized, Controlled, and Open-Label Study. International journal of general medicine, 14, 2359–2366. https://doi.org/10.2147/IJGM.S318720
[29]Wong, Y., Chan, C. H., Venkatakrishnan, K., Chiu, H. F., Shen, Y. C., Glovinskaia, O., ... & Wang, C. K. (2021). Impact of dietary nutrients (functional foods/nutraceuticals) and micronutrients on COVID-19: A review. Journal of Food Bioactives, 15.
[30]Martineau, A. R., Jolliffe, D. A., Hooper, R. L., Greenberg, L., Aloia, J. F., Bergman, P., Dubnov-Raz, G., Esposito, S., Ganmaa, D., Ginde, A. A., Goodall, E. C., Grant, C. C., Griffiths, C. J., Janssens, W., Laaksi, I., Manaseki-Holland, S., Mauger, D., Murdoch, D. R., Neale, R., Rees, J. R., … Camargo, C. A., Jr (2017). Vitamin D supplementation to prevent acute respiratory tract infections: systematic review and meta-analysis of individual participant data. BMJ (Clinical research ed.), 356, i6583. https://doi.org/10.1136/bmj.i6583
[31]Meltzer, D. O., Best, T. J., Zhang, H., Vokes, T., Arora, V., & Solway, J. (2020). Association of Vitamin D Status and Other Clinical Characteristics With COVID-19 Test Results. JAMA network open, 3(9), e2019722. https://doi.org/10.1001/jamanetworkopen.2020.19722
[32]Wintergerst, E. S., Maggini, S., & Hornig, D. H. (2006). Immune-enhancing role of vitamin C and zinc and effect on clinical conditions. Annals of nutrition & metabolism, 50(2), 85–94. https://doi.org/10.1159/000090495
[33]Tomasa-Irriguible, T. M., & Bielsa-Berrocal, L. (2021). COVID-19: Up to 82% critically ill patients had low Vitamin C values. Nutrition journal, 20(1), 66. https://doi.org/10.1186/s12937-021-00727-z
[34]Hemilä, H., Carr, A., & Chalker, E. (2021). Vitamin C May Increase the Recovery Rate of Outpatient Cases of SARS-CoV-2 Infection by 70%: Reanalysis of the COVID A to Z Randomized Clinical Trial. Frontiers in immunology, 12, 674681. https://doi.org/10.3389/fimmu.2021.674681
[35]Hunter, J., Arentz, S., Goldenberg, J., Yang, G., Beardsley, J., Myers, S. P., Mertz, D., & Leeder, S. (2021). Zinc for the prevention or treatment of acute viral respiratory tract infections in adults: a rapid systematic review and meta-analysis of randomised controlled trials. BMJ open, 11(11), e047474. https://doi.org/10.1136/bmjopen-2020-047474
[36]Louca, P., Murray, B., Klaser, K., Graham, M. S., Mazidi, M., Leeming, E. R., Thompson, E., Bowyer, R., Drew, D. A., Nguyen, L. H., Merino, J., Gomez, M., Mompeo, O., Costeira, R., Sudre, C. H., Gibson, R., Steves, C. J., Wolf, J., Franks, P. W., Ourselin, S., … Menni, C. (2021). Modest effects of dietary supplements during the COVID-19 pandemic: insights from 445 850 users of the COVID-19 Symptom Study app. BMJ nutrition, prevention & health, 4(1), 149–157. https://doi.org/10.1136/bmjnph-2021-000250
[37]Shakoor, H., Feehan, J., Mikkelsen, K., Al Dhaheri, A. S., Ali, H. I., Platat, C., Ismail, L. C., Stojanovska, L., & Apostolopoulos, V. (2021). Be well: A potential role for vitamin B in COVID-19. Maturitas, 144, 108–111. https://doi.org/10.1016/j.maturitas.2020.08.007
[38]Calder P. C. (2020). Nutrition, immunity and COVID-19. BMJ nutrition, prevention & health, 3(1), 74–92. https://doi.org/10.1136/bmjnph-2020-000085
[39]http://www.nhc.gov.cn/ylyjs/pqt/202212/2b6c16cc176b4806b399ea5588353b3c.shtm
[40]https://mp.weixin.qq.com/s/x4LCCyOcU1o2_EOFIDsnBw
[41]Luo, P., Qiu, L., Liu, Y., Liu, X. L., Zheng, J. L., Xue, H. Y., Liu, W. H., Liu, D., & Li, J. (2020). Metformin Treatment Was Associated with Decreased Mortality in COVID-19 Patients with Diabetes in a Retrospective Analysis. The American journal of tropical medicine and hygiene, 103(1), 69–72. https://doi.org/10.4269/ajtmh.20-0375
[42]Ursini, F., Russo, E., Pellino, G., D'Angelo, S., Chiaravalloti, A., De Sarro, G., Manfredini, R., & De Giorgio, R. (2018). Metformin and Autoimmunity: A "New Deal" of an Old Drug. Frontiers in immunology, 9, 1236. https://doi.org/10.3389/fimmu.2018.01236
[43]Bendib, I., de Chaisemartin, L., Granger, V., Schlemmer, F., Maitre, B., Hüe, S., Surenaud, M., Beldi-Ferchiou, A., Carteaux, G., Razazi, K., Chollet-Martin, S., Mekontso Dessap, A., & de Prost, N. (2019). Neutrophil Extracellular Traps Are Elevated in Patients with Pneumonia-related Acute Respiratory Distress Syndrome. Anesthesiology, 130(4), 581–591. https://doi.org/10.1097/ALN.0000000000002619
[44]Zheng, M., Schultz, M. B., & Sinclair, D. A. (2022). NAD+ in COVID-19 and viral infections. Trends in immunology, 43(4), 283–295. https://doi.org/10.1016/j.it.2022.02.001
[45]Jiang, Y., Deng, Y., Pang, H., Ma, T., Ye, Q., Chen, Q., Chen, H., Hu, Z., Qin, C. F., & Xu, Z. (2022). Treatment of SARS-CoV-2-induced pneumonia with NAD+ and NMN in two mouse models. Cell discovery, 8(1), 38. https://doi.org/10.1038/s41421-022-00409-y
[46]Zuo, Y., Yalavarthi, S., Shi, H., Gockman, K., Zuo, M., Madison, J. A., Blair, C., Weber, A., Barnes, B. J., Egeblad, M., Woods, R. J., Kanthi, Y., & Knight, J. S. (2020). Neutrophil extracellular traps in COVID-19. JCI insight, 5(11), e138999. https://doi.org/10.1172/jci.insight.138999
[47]Bonetti, G., Medori, M. C., Fioretti, F., Farronato, M., Nodari, S., Lorusso, L., Tartaglia, G. M., Farronato, G., Bellinato, F., Gisondi, P., Connelly, S. T., & Bertelli, M. (2022). Dietary supplements for the management of COVID-19 symptoms. Journal of preventive medicine and hygiene, 63(2 Suppl 3), E221–E227. https://doi.org/10.15167/2421-4248/jpmh2022.63.2S3.2764
[48]Bath, P. M., Skinner, C. J. C., Bath, C. S., Woodhouse, L. J., Korovesi, A. A. K., Long, H., Havard, D., Coleman, C. M., England, T. J., Leyland, V., Lim, W. S., Montgomery, A. A., Royal, S., Avery, A., Webb, A. J., Gordon, A. L., & for BEET-Winter Investigators (2022). Dietary nitrate supplementation for preventing and reducing the severity of winter infections, including COVID-19, in care homes (BEET-Winter): a randomised placebo-controlled feasibility trial. European geriatric medicine, 13(6), 1343–1355. https://doi.org/10.1007/s41999-022-00714-5
[49]https://mp.weixin.qq.com/s?__biz=Mzg5MDU0NTQ4NA==&mid=2247509827&idx=1&sn=7f1ea0bc36b8c13b471e9ee92da930eb&chksm=cfd81360f8af9a76c058dea535858b26467b0e6fffa482991ab5cb65fc03b497cccc4383a949&token=348783477&lang=zh_CN#rd
[50]https://mp.weixin.qq.com/s?__biz=Mzg5MDU0NTQ4NA==&mid=2247509777&idx=1&sn=023cd5b673de36799e5546f5eb25e788&chksm=cfd81332f8af9a24653eb04e4b837d87e454480f04d765f3db7485dc23b9d7a73dd2b08c0313&token=348783477&lang=zh_CN#rd
[51]https://mp.weixin.qq.com/s?__biz=Mzg5MDU0NTQ4NA==&mid=2247510135&idx=1&sn=fac05ea1febf21869323353904ab9f81&chksm=cfd81c54f8af954299c3ec8cef904f5101aa7ba4552c49170d7c7c0ff3a843f64c6b857df1fd&token=348783477&lang=zh_CN#rd
[52]https://mp.weixin.qq.com/s?__biz=Mzg5MDU0NTQ4NA==&mid=2247509858&idx=1&sn=34c8f4c799f7d150fc66ba4f10431c9d&chksm=cfd81341f8af9a57361e50b1147a413113b1c5553de620127bfbc9b7b162af3c5fca606f5448&token=348783477&lang=zh_CN#rd
[53]Soriano, J. B., Murthy, S., Marshall, J. C., Relan, P., Diaz, J. V., & WHO Clinical Case Definition Working Group on Post-COVID-19 Condition (2022). A clinical case definition of post-COVID-19 condition by a Delphi consensus. The Lancet. Infectious diseases, 22(4), e102–e107. https://doi.org/10.1016/S1473-3099(21)00703-9
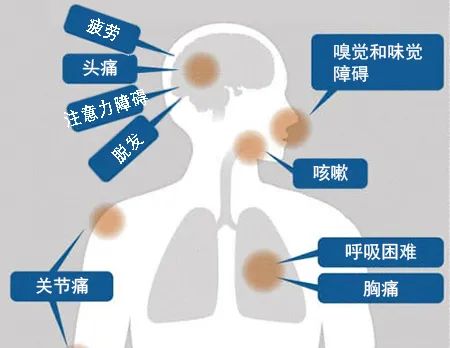
[54]Lopez-Leon, S., Wegman-Ostrosky, T., Perelman, C., Sepulveda, R., Rebolledo, P. A., Cuapio, A., & Villapol, S. (2021). More than 50 long-term effects of COVID-19: a systematic review and meta-analysis. Scientific reports, 11(1), 16144. https://doi.org/10.1038/s41598-021-95565-8
[55]Dumont, R., Richard, V., Lorthe, E., Loizeau, A., Pennacchio, F., Zaballa, M. E., Baysson, H., Nehme, M., Perrin, A., L'Huillier, A. G., Kaiser, L., Barbe, R. P., Posfay-Barbe, K. M., Stringhini, S., SEROCoV-KIDS study group, & Guessous, I. (2022). A population-based serological study of post-COVID syndrome prevalence and risk factors in children and adolescents. Nature communications, 13(1), 7086. https://doi.org/10.1038/s41467-022-34616-8
[56]Greenhalgh, T., Knight, M., A'Court, C., Buxton, M., & Husain, L. (2020). Management of post-acute covid-19 in primary care. BMJ (Clinical research ed.), 370, m3026. https://doi.org/10.1136/bmj.m3026
[57]https://www.cdc.gov/coronavirus/2019-ncov/hcp/clinical-care/post-covid-conditions.html?CDC_AA_refVal=https%3A%2F%2Fwww.cdc.gov%2Fcoronavirus%2F2019-ncov%2Fhcp%2Fclinical-care%2Fpost-covid-management.html
[58]Rossi Ferrario, S., Panzeri, A., Cerutti, P., & Sacco, D. (2021). The Psychological Experience and Intervention in Post-Acute COVID-19 Inpatients. Neuropsychiatric disease and treatment, 17, 413–422. https://doi.org/10.2147/NDT.S283558
[59]https://www.england.nhs.uk/coronavirus/publication/pulse-oximetry-to-detect-early-deterioration-of-patients-with-covid-19-in-primary-and-community-care-settings/
[60]Vollbracht, C., & Kraft, K. (2021). Feasibility of Vitamin C in the Treatment of Post Viral Fatigue with Focus on Long COVID, Based on a Systematic Review of IV Vitamin C on Fatigue. Nutrients, 13(4), 1154. https://doi.org/10.3390/nu13041154
[61]Jarrott, B., Head, R., Pringle, K. G., Lumbers, E. R., & Martin, J. H. (2022). "LONG COVID"-A hypothesis for understanding the biological basis and pharmacological treatment strategy. Pharmacology research & perspectives, 10(1), e00911. https://doi.org/10.1002/prp2.911
[62]Robbins, T., Gonevski, M., Clark, C., Baitule, S., Sharma, K., Magar, A., Patel, K., Sankar, S., Kyrou, I., Ali, A., & Randeva, H. S. (2021). Hyperbaric oxygen therapy for the treatment of long COVID: early evaluation of a highly promising intervention. Clinical medicine (London, England), 21(6), e629–e632. https://doi.org/10.7861/clinmed.2021-0462
[63]Karosanidze, I., Kiladze, U., Kirtadze, N., Giorgadze, M., Amashukeli, N., Parulava, N., Iluridze, N., Kikabidze, N., Gudavadze, N., Gelashvili, L., Koberidze, V., Gigashvili, E., Jajanidze, N., Latsabidze, N., Mamageishvili, N., Shengelia, R., Hovhannisyan, A., & Panossian, A. (2022). Efficacy of Adaptogens in Patients with Long COVID-19: A Randomized, Quadruple-Blind, Placebo-Controlled Trial. Pharmaceuticals (Basel, Switzerland), 15(3), 345. https://doi.org/10.3390/ph15030345
[64]Zhou, X., Yang, D., Kong, X., Wei, C., LvQiu, S., Wang, L., Lin, Y., Yin, Z., Zhou, Z., & Luo, H. (2022). Case Report: Pirfenidone in the Treatment of Post-COVID-19 Pulmonary Fibrosis. Frontiers in medicine, 9, 925703. https://doi.org/10.3389/fmed.2022.925703
[65]https://clinicaltrials.gov/ct2/show/NCT04695704
[66]https://clinicaltrials.gov/ct2/show/NCT04809974
[67]Gaylis, N. B., Ritter, A., Kelly, S. A., Pourhassan, N. Z., Tiwary, M., Sacha, J. B., Hansen, S. G., Recknor, C., & Yang, O. O. (2022). Reduced Cell Surface Levels of C-C Chemokine Receptor 5 and Immunosuppression in Long Coronavirus Disease 2019 Syndrome. Clinical infectious diseases : an official publication of the Infectious Diseases Society of America, 75(7), 1232–1234. https://doi.org/10.1093/cid/ciac226
[68]Crook, H., Raza, S., Nowell, J., Young, M., & Edison, P. (2021). Long covid-mechanisms, risk factors, and management. BMJ (Clinical research ed.), 374, n1648. https://doi.org/10.1136/bmj.n1648
[69]Deng, L., Li, P., Zhang, X., Jiang, Q., Turner, D., Zhou, C., Gao, Y., Qian, F., Zhang, C., Lu, H., Zou, H., Vermund, S. H., & Qian, H. Z. (2022). Risk of SARS-CoV-2 reinfection: a systematic review and meta-analysis. Scientific reports, 12(1), 20763. https://doi.org/10.1038/s41598-022-24220-7
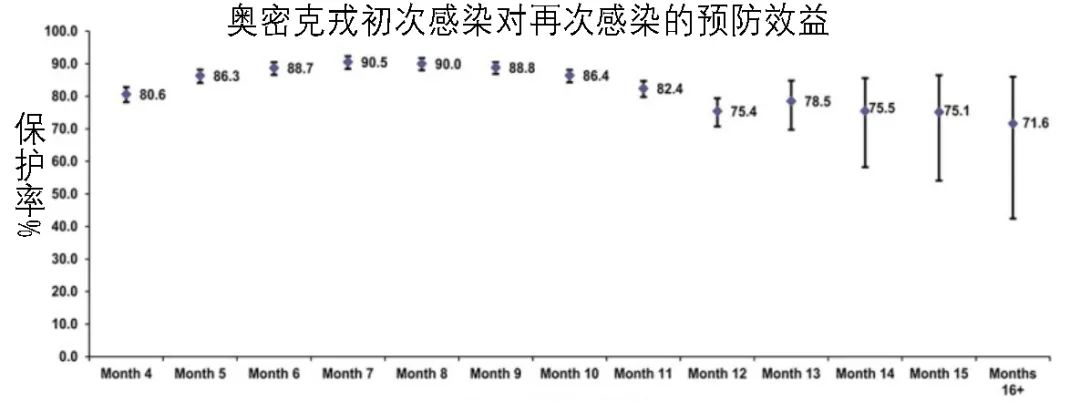
[70]Chemaitelly, H., Nagelkerke, N., Ayoub, H. H., Coyle, P., Tang, P., Yassine, H. M., Al-Khatib, H. A., Smatti, M. K., Hasan, M. R., Al-Kanaani, Z., Al-Kuwari, E., Jeremijenko, A., Kaleeckal, A. H., Latif, A. N., Shaik, R. M., Abdul-Rahim, H. F., Nasrallah, G. K., Al-Kuwari, M. G., Butt, A. A., Al-Romaihi, H. E., … Abu-Raddad, L. J. (2022). Duration of immune protection of SARS-CoV-2 natural infection against reinfection. Journal of travel medicine, taac109. Advance online publication. https://doi.org/10.1093/jtm/taac109
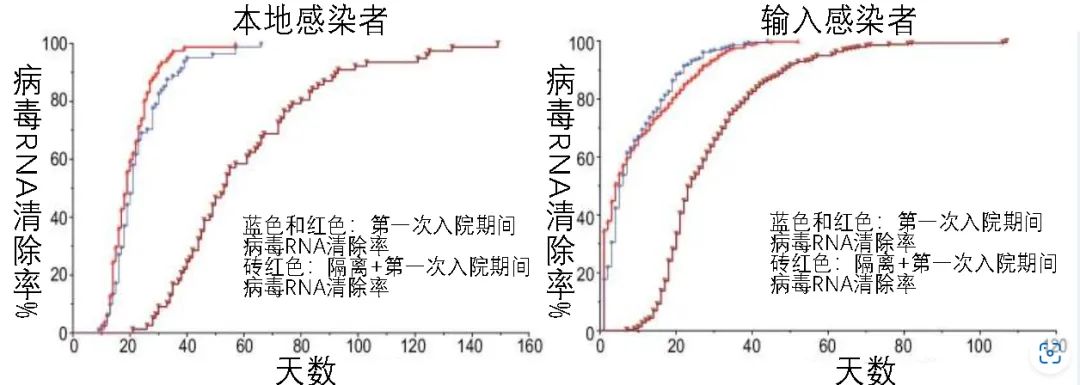
[71]Li, L., Tang, J., Xie, Z., Gan, Q., Tang, G., Hu, Z., Zeng, H., Shi, J., Li, J., Li, Y., Ke, C., Kang, M., Liang, D., Lu, H., Tong, Y., Deng, X., Liu, J., Lu, H., Wang, F., Hu, F., … Tang, X. (2022). Characteristics of SARS-CoV-2 Delta variant-infected individuals with intermittently positive retest viral RNA after discharge. National science review, 9(10), nwac141. https://doi.org/10.1093/nsr/nwac141
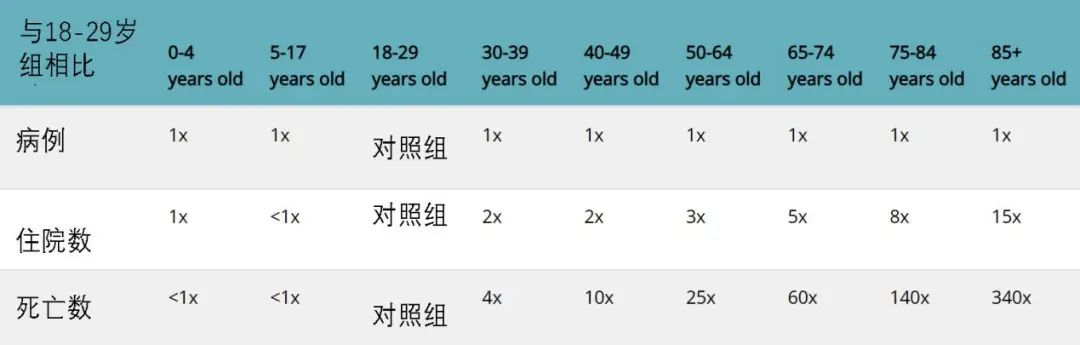
[72]https://www.cdc.gov/coronavirus/2019-ncov/hcp/clinical-care/underlyingconditions.html
[73]Tehrani, S., Killander, A., Åstrand, P., Jakobsson, J., & Gille-Johnson, P. (2021). Risk factors for death in adult COVID-19 patients: Frailty predicts fatal outcome in older patients. International journal of infectious diseases : IJID : official publication of the International Society for Infectious Diseases, 102, 415–421. https://doi.org/10.1016/j.ijid.2020.10.071
[74]Cheung, P. H., Chan, C. P., & Jin, D. Y. (2022). Lessons learned from the fifth wave of COVID-19 in Hong Kong in early 2022. Emerging microbes & infections, 11(1), 1072–1078. https://doi.org/10.1080/22221751.2022.2060137
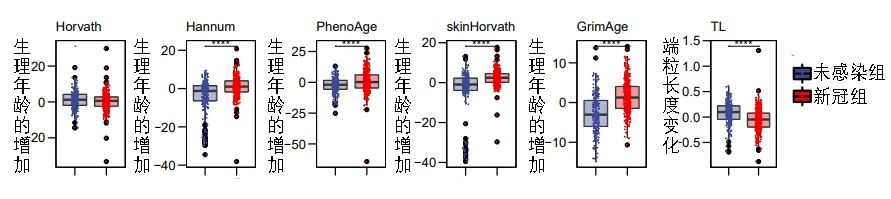
[75]Cao, X., Li, W., Wang, T., Ran, D., Davalos, V., Planas-Serra, L., Pujol, A., Esteller, M., Wang, X., & Yu, H. (2022). Accelerated biological aging in COVID-19 patients. Nature Communications, 13(1). https://doi.org/10.1038/s41467-022-29801-8
[76]Sila, T., Sunghan, J., Laochareonsuk, W., Surasombatpattana, S., Kongkamol, C., Ingviya, T., Siripaitoon, P., Kositpantawong, N., Kanchanasuwan, S., Hortiwakul, T., Charernmak, B., Nwabor, O. F., Silpapojakul, K., & Chusri, S. (2022). Suspected Cat-to-Human Transmission of SARS-CoV-2, Thailand, July-September 2021. Emerging infectious diseases, 28(7), 1485–1488. https://doi.org/10.3201/eid2807.212605
[77]Yen, H. L., Sit, T. H. C., Brackman, C. J., Chuk, S. S. Y., Gu, H., Tam, K. W. S., Law, P. Y. T., Leung, G. M., Peiris, M., Poon, L. L. M., & HKU-SPH study team (2022). Transmission of SARS-CoV-2 delta variant (AY.127) from pet hamsters to humans, leading to onward human-to-human transmission: a case study. Lancet (London, England), 399(10329), 1070–1078. https://doi.org/10.1016/S0140-6736(22)00326-9
[78]Öcal, D. F., Öztürk, F. H., Şenel, S. A., Sinaci, S., Yetişkin, F. D. Y., Keven, C., Dinç, B., Turgut, E., Oluklu, D., Tekin, Ö. M., & Şahin, D. (2022). The influence of COVID-19 pandemic on intrauterine fetal demise and possible vertical transmission of SARS-CoV-2. Taiwanese journal of obstetrics & gynecology, 61(6), 1021–1026. https://doi.org/10.1016/j.tjog.2022.03.047
[79]Asalkar, M. R., Thakkarwad, S. M., Bacchewad, R. P., & Sharma, N. H. (2022). Perinatal Outcome in Maternal COVID-19 infection at a Tertiary care Institute- A cross Sectional Study. Journal of obstetrics and gynaecology of India, 1–9. Advance online publication. https://doi.org/10.1007/s13224-022-01673-4
[80]Calabretto, M., D'Alisa, R., Faraone, S., Mazzuti, L., Pecorini, F., & Turriziani, O. (2022). Detection of SARS-CoV-2 RNA and antibodies in breast milk of infected mothers. Journal of medical virology, 10.1002/jmv.28142. Advance online publication. https://doi.org/10.1002/jmv.28142
[81]Anto-Ocrah, M., Valachovic, T., Chen, M., Tiffany, K., DeSplinter, L., Kaukeinen, K., Glantz, J. C., & Hollenbach, S. (2022). Coronavirus Disease 2019 (COVID-19)-Related Stress and Menstrual Changes. Obstetrics and gynecology, 10.1097/AOG.0000000000005010. Advance online publication. https://doi.org/10.1097/AOG.0000000000005010
[82]Male V. (2022). COVID-19 vaccination and menstruation. Science (New York, N.Y.), 378(6621), 704–706. https://doi.org/10.1126/science.ade1051
[83]Lazarus, J. V., Romero, D., Kopka, C. J., Karim, S. A., Abu-Raddad, L. J., Almeida, G., Baptista-Leite, R., Barocas, J. A., Barreto, M. L., Bar-Yam, Y., Bassat, Q., Batista, C., Bazilian, M., Chiou, S. T., Del Rio, C., Dore, G. J., Gao, G. F., Gostin, L. O., Hellard, M., Jimenez, J. L., … COVID-19 Consensus Statement Panel (2022). A multinational Delphi consensus to end the COVID-19 public health threat. Nature, 611(7935), 332–345. https://doi.org/10.1038/s41586-022-05398-2